2022 Validation Report
Review for: Nova Healthcare Administrators
Validation Achieved: Outcomes
Savings Valid Through: January 2023
Company Profile
Category:
Third Party Administrator
Website:
Public or Private:
Private
Year Established:
1982
President:
James Walleshauser
Company Contact:
Description:
Evolving over the last 30 years, Nova aims to manage trend to reduce health care spend and improve health plan performance. Headquartered in Buffalo, NY, Nova is a wholly-owned affiliate of Independent Health.
Nova works with flexibility to provide the solutions clients need in the way clients need them including medical, dental, vision, COBRA, reimbursement account administration, and private-labeled partnerships. Nova provides clients with unique cost management and customized health plan strategies through personalized service.
Claim Assertion
Nova creates a cost and risk management strategy tailored to each employer’s benefit plan, culture, and goals. The strategy uses medical, behavioral, and pharmacy claims, plus operational observations, a company-level assessment and lab data (when available). The strategy addresses preventive care, early detection of illness, improving treatment compliance, appropriateness of services, and reducing cost of necessary care. Nova’s clients have had annual rate increases that are lower by half than a national benchmark.
In 2020, Nova has once again achieved below-average admissions and emergency room visits for common chronic disease.
Method/Calculation/Examples
Member-facing validations are done using the “gold standard” event rate tracking methodology. This is the only metric which avoids participant bias, regression to the mean, and trend inflation, three invalidators detailed respectively in those links. This methodology, invented by the founders of the Validation Institute, has been accepted and published by Health Affairs and the Health Enhancement Research Organization. It has also been featured in Why Nobody Believes the Numbers: Distinguishing Fact from Fiction in Population Health Management, the award-winning trade-bestselling textbook most widely used among professional and graduate programs in population health outcomes measurement. It is also the only methodology which qualifies for the Validation Institute’s Credibility Guarantee for member-facing programs. Details include:
•Uses very specific ICD-10s
•No regression to the mean
•Age taken into account
•All data submission is QC’ed
•Only valid methodology in use
Findings & Validation
The validation itself is for the measurement itself. Whether the validated organization has achieved better-than-average outcomes is mentioned in the member-specific language and is viewable in the attached slides. (It will appear that most validated organizations have indeed achieved better-than-average outcomes. That is because other organizations prefer not to be posted.). ROIs are not listed because the ROI will depend on the price charged. In order to achieve a positive ROI, an organization must keep events below the benchmark. However, not every organization outperforming the benchmark will achieve a positive ROI.
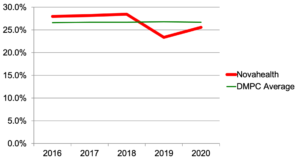
Figure 1: Aging comparison: Nova vs. DMPC database percentage of members 50 to 64.9 years old
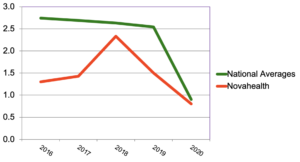
Figure 2: Asthma vs. national averages (events per 1000 ASO members)
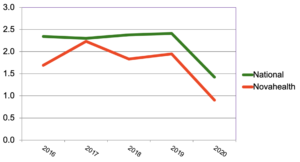
Figure 3: CAD vs. national averages (events per 1000 ASO members)
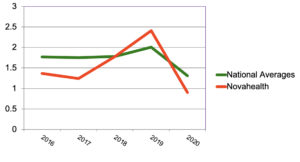
Figure 4: CHF/HTN vs. national averages (events per 1000 ASO members)
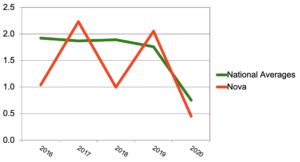
Figure 5: COPD vs. national averages (events per 1000 ASO members)
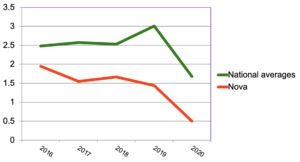
Figure 6: Diabetes vs. national averages (events per 1000 ASO members)
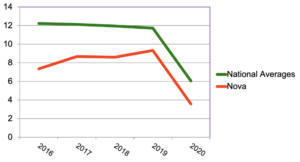
Figure 7: Total Events vs. national averages (events per 1000 ASO members)
Limitations
While all event rates fell in 2020, Nova’s declined more than most.
Validation and Credibility Guarantee
Nova Healthcare Administrators achieved validation for Outcomes. Validation Institute is willing to provide up to a $25,000 guarantee as part of their Credibility Guarantee Program. To learn more, visit https://validationinstitute.com/credibility-guarantee/.
Program Validation
Program has strong evidence of significant impact on both patient outcomes and on medical costs. Evidence is assessed based upon the certainty it provides that the result is due to the program and not to other factors, such as recruiting people to participate in the program who are most likely to succeed.
Savings
Can reduce health care spending per case/participant or for the plan/purchaser overall.
Outcomes
Product/solution has measurably improved an outcome (risk, hba1c, events, employee retention, etc.) of importance.
Metrics
Credible sources and valid assumptions create a reasonable estimate of a program’s impact.
Contractual Integrity
Vendor is willing to put a part of their fees "at risk" as a guarantee.
About Validation Institute
Validation Institute is a professional community that advocates for organizations and approaches that deliver better health value - stronger health outcomes at lower cost. We connect, train, and certify health care purchasers, and we validate and connect providers delivering superior results. Founded in 2014, the mission of the organization has consistently been to help provide transparency to buyers of health care.
Validation Review ProcessValidation Institute has a team of epidemiologists and statisticians who review each program. The team focuses on three components:
- Evidence from published literature that a similar intervention had similar results.
- The reliability and credibility of the data sources.
- The rigor of the approach to calculating results
To achieve validation, the program has to satisfy each of these components. VI’s team then summarizes the review into a report which is publicly available. Details of VI’s review are available with the program’s permission.